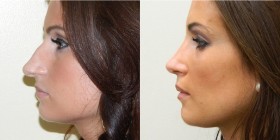
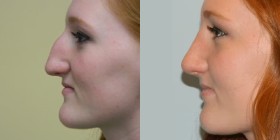
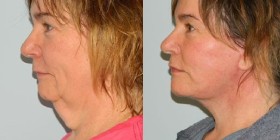
Rhinoplasty, commonly referred to as a nose job, is any surgery done to change the shape of the nose. Rhinoplasty may be done for purely cosmetic reasons, for purely functional reasons such as to improve nasal breathing, or a combination of the two.
Because the nose has a very prominent central location on the face, the changes made with rhinoplasty can make a dramatic difference in a person’s appearance and lead to great increases in self-esteem and self-confidence.
Cosmetic rhinoplasty can change an almost infinite number of variations in nasal shapes. The goal of the surgery is to give an improved nasal contour that is in harmony with the rest of the face, while maintaining or improving nasal breathing. Most often, rhinoplasty is done to make a large nose smaller or a wide nose narrower, but occasionally the opposite is true.
Contents
The Consultation
Anyone considering rhinoplasty should see a board-certified facial plastic surgeon, otolaryngologist/head and neck surgeon (ENT), or general plastic surgeon for a consultation. The patient should seek out a surgeon who has extensive training and experience with both the cosmetic and functional aspects of this operation. It is advisable to ask to see a portfolio of before-and-after photographs of other rhinoplasties the surgeon has performed.
The consultation is an opportunity for me to listen to patients’ goals, to examine them, and to come up with a surgical plan. I examine the external and internal nose to determine what changes are possible. It is very helpful for patients to be able to clearly express what they do not like about their noses so I can determine if their goals are realistic. I also attempt to explore exactly what a patient’s motivation is for wanting nasal surgery. It is important to make sure that the patient has carefully thought about the decision to have surgery and that the desire is not based on a whim, to please someone else, or because of a recent life-changing event, such as a divorce.
During the consultation, I use computer imaging to show patients the changes that are possible. Computer imaging is a powerful tool that is useful in establishing clear communication between the patient and myself as to what the surgical goal should be. It is important to note, however, that the computer-simulated photographs are only an estimation of the desired outcome. Although the actual result of surgery usually closely approximates the computer-simulated images, no surgeon can guarantee to what extent a complete match will occur.
Assessing the Face
When examining the patient, I look at the entire face to determine what changes are needed to create the most aesthetically pleasing result. I take into account the patient’s ethnic background, bony and cartilaginous anatomy, skin thickness, general health status, and age. Female patients should be at least 15 to 16 years old and males should be 16 to 17 years old—ages at which the vast majority of nasal growth has been completed. Nasal surgery done prior to the completion of nasal growth may result in developmental abnormalities of the nose.
At the consultation I may also suggest that the patient undergo another procedure in combination with the rhinoplasty to maximize facial harmony and balance. The most common procedure done in combination with rhinoplasty is chin augmentation, but cheek augmentation and chin reduction may also be done in combination with rhinoplasty.
Surgery location
The rest of my consultation includes a discussion of the different locations at which I perform surgery. These locations include hospital operating rooms, surgicenters, and my office operating rooms. Patients should be sure that anesthesia given in an office operating room is provided by a licensed anesthesiologist or nurse anesthetist. Also, all of the same monitoring equipment present in a hospital operating room, such as EKG machines and blood-oxygen level monitors, should be in the office for your surgery.
Patients are usually given local anesthesia with sedation to place them in a comfortable drowsy state, but they remain awake. The other option is general anesthesia where the patient goes to sleep fully. The first option is safer and has less postoperative nausea and a quicker recovery.
Rhinoplasty Techniques
There is a multitude of variations in rhinoplasty techniques. The technique used depends on what type of problem exists and also on the individual surgeon’s preference. Most of the incisions are placed inside the nose, but some surgeons employ a technique called open or external rhinoplasty, in which a small incision is placed in the columella, which is the bridge of skin separating the two nostrils. This incision, when connected with the intranasal incisions, allows better exposure of the nasal anatomy than the more traditional techniques. The benefits of improved exposure are better symmetry and more sophisticated ways of altering the nasal anatomy, which I believe lead to better results. Also, occasionally, incisions are placed at the base of the nostrils for nostril narrowing.
Bone restructuring
Once the surgical exposure of the cartilage and bones of the nose is accomplished, many different maneuvers are used to modify them.
Nasal bones and cartilage may be shaved down if too prominent, repositioned if out of alignment or too wide, or added to if deficient. Nasal tip cartilages are often reduced in size and sutures are placed to narrow and refine them.
Often, in the case of twisted, deviated, or wide noses, cuts will be made in the nasal bones to allow them to be repositioned. Deficiencies in the nasal structure are replaced with grafts of cartilage from the nasal septum, ear or rib, or bone from the skull, rib, or hip. Nasal deficiencies may also be replaced with synthetic materials such as Gore-TexTM or SilasticTM. The advantage of using synthetic materials for nasal augmentation is that no further surgical procedures are needed to harvest these materials. The implant is simply removed from a sterile package, carved to the proper shape and implanted. The disadvantage of synthetic implants is that they can become infected or lead to thinning of the skin and eventual exposure of the implant necessitating implant removal. Implants from the patient’s own cartilage or bone almost never cause any of these problems.
After all of the modifications to the nasal structure are completed the incisions are closed and a cast is usually applied. Occasionally, depending on exactly what type of procedure was done, VaselineTM gauze or a sponge dressing may be placed inside the nose for one to two days.
What to Expect After Surgery
After surgery, patients usually have minimal pain, which is easily controlled with pain medication. The degree of swelling and bruising depends on how extensive the surgery was. If mobilizing and repositioning the nasal bones was not part of the surgery then swelling and bruising around the eyes is usually minimal. If the nasal bones were repositioned, swelling and bruising around the eyes may be significant, but is usually gone in seven-to-ten days. Most patients feel comfortable going out in public by this time. Some surgeons give steroid medications for a few days after the surgery in an attempt to minimize swelling as much as possible. By six weeks, the majority of swelling of the nose is gone, but it often takes many months for the final amounts of swelling to disappear.
Sleeping
It is helpful for the patient to sleep with his or her head elevated on a few pillows for the first week to allow gravity to aid in reducing the swelling as quickly as possible. The cast is usually removed after one week and any external sutures that were used are also removed around this time. When the cast is removed, the patient will get some idea of how the nose will look, but during the next few weeks to months, significant changes will occur with healing and the disappearance swelling.
Post-surgery activities
Patients are told not to engage in any strenuous activities for the first two weeks after surgery that could lead to nose bleeds, and to avoid direct sun exposure for the first few months, which would lead to swelling of the nose. Also, it is advisable for the first six weeks to avoid activities that could lead to the nose being hit or bumped. Patients who wear glasses may be advised to tape their glasses to their foreheads for a few weeks if their nasal bones were repositioned in order to avoid the weight of the glasses displacing the nasal bones.
Surgical Risks
All surgery is associated with risks. For patients who do not have significant medical problems, the risks are minimal. Any surgery can result in an infection, a bleeding problem, or an adverse reaction to the anesthesia medications. Again, these are extremely rare occurrences. Poor healing, the development of scar tissue under the skin, nasal contour irregularities and postoperative nasal breathing problems are also possible occurrences. All of these complications are treatable.
Surgical Costs
The surgical fee for rhinoplasty varies from doctor to doctor and may depend on how extensive the surgery will be, but a range of $3,000 to $5,000 is typical. Insurance may cover the entire cost of the surgery including anesthesia and operating room fees if the surgery is done for functional and not cosmetic reasons. Rhinoplasty, for a combination of functional and cosmetic reasons, may be partially covered, but surgery for purely cosmetic reasons is not covered by insurance.
Conclusion
The latest techniques used in rhinoplasty allow surgeons to give patients natural, aesthetically pleasing results with good nasal function. Patients with the proper self-motivation and realistic expectations for the surgery are usually very pleased.